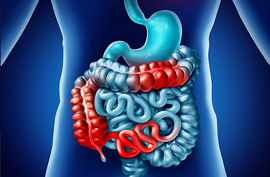
What is Crohn's disease?
Crohn’s disease is a chronic inflammatory condition affecting any part of your gastrointestinal tract from the mouth to the anus. Most commonly affected are the large intestine (colon) and the end of the small intestine (terminal ileum).
What causes Crohn’s disease?
The exact cause of Crohn’s disease is not well understood. Crohn’s disease causes uncontrolled inflammation within the digestive tract. There are autoimmune, genetic and environmental factors implicated, but no single cause has been established. The theory is that the immune system of the digestive tract is activated in the setting of something foreign, referred to as an antigen. In Crohn’s disease, once activated, the immune system of the digestive is unable to “turn off” and as a result unregulated inflammation occurs.
Who is affected?
Crohn’s disease occurs equally in men and women. The disease is more common in caucasians but seen amongst all races and ethnicities. Those with a family history of inflammatory bowel disease may be at an increased risk. The disease is often diagnosed in adolescents and adults between the ages of 20 and 30; however, it can occur at any age.
What are the symptoms of Crohn’s disease?
The symptoms of Crohn’s disease are variable and depend on where the inflammation is occurring and the extent of that inflammation. Common symptoms include diarrhea, abdominal pain and weight loss. Gastrointestinal bleeding can occur but is more commonly seen in ulcerative colitis. More severe disease can lead to fistulas (tunnels between the intestines, internal organs and skin) and intestinal strictures (narrowings). Patients may have signs and symptoms of vitamin and nutrient deficiencies. Furthermore, Crohn’s disease can involve the anal area and cause anal pain, tears, fistulas (tunnels between skin and internal organs), infections and narrowings. Outside the gastrointestinal tract, Crohn’s disease can be associated with joint inflammation (arthritis), redness or pain in the eyes and mouth sores, among others.
Overall, Crohn’s symptoms can range from no symptoms at all to severe, highly complex disease. It is a chronic condition for which there is no cure. Patient’s symptoms can be episodic and occur in flares, during which time their disease is active and may require more aggressive therapy.
How is Crohn’s disease diagnosed?
There is no single test to diagnose Crohn’s disease. The diagnosis of Crohn’s relies on a combination of a detailed history, physical exam findings, labs, stool testing, endoscopy, colonoscopy, small bowel capsule endoscopy and imaging.
How is Crohn’s disease treated?
The goal of treatment in Crohn’s disease is to achieve a state of remission (no disease activity). This is done using a combination of treatment options and depends largely on the severity, disease location and other medical conditions you may have. Medical treatments aim to control inflammation and stop further intestinal damage. Some of the medicines used in Crohn’s disease include:
• Steroids - These include prednisone, methylprednisolone and budesonide. These medications are used in the acute setting to get control of inflammation but are not recommended in the long-term due to side effects.
• 5-Aminosalicylates (5-ASA) - This group of medicines have anti-inflammatory effects on the intestines. They are more beneficial in the treatment of ulcerative colitis but are at times used as an alternative therapy in mildly active Crohn’s disease.
• Immunomodulators - These medications are used in patients with more severe disease not responding to steroids or 5-ASAs. They work by suppressing the body’s immune system to control the inflammation seen in Crohn’s.
• Biologics - These medications are used in the patients who have not responded to conventional therapy. They are antibodies that are directed against certain proteins within the body that cause inflammation. Examples include Adalimumab (Humira®), Certolizumab pegol (Cimzia®), Infliximab (Remicade®), Ustekinumab (Stelara®) and Vedolizumab (Entyvio®).
Surgery for Crohn’s Disease
Medications are used to control the disease activity of Crohn’s and prevent any complications as a result of uncontrolled inflammation. Despite medical treatment, about 80 percent of patients with Crohn’s will require some type of surgery in their lifetime. Surgery does not cure Crohn’s disease but it can help improve symptoms and overall quality of life.
The information provided above is meant to be used as an informative guide for patients. For precise and individualized recommendations, please consult with one of our board certified gastroenterologists to discuss your symptoms.
For additional information or to book an appointment at the Gastroenterology Center of New York, please feel free to reach out to our dedicated team by calling us at 718-210-2960. You can also schedule online or reach out to us via the Contact Us form.
Questions? Our staff is always happy to assist.
Email us at info@gastrocenterofny.com or call us at 718.210.2960